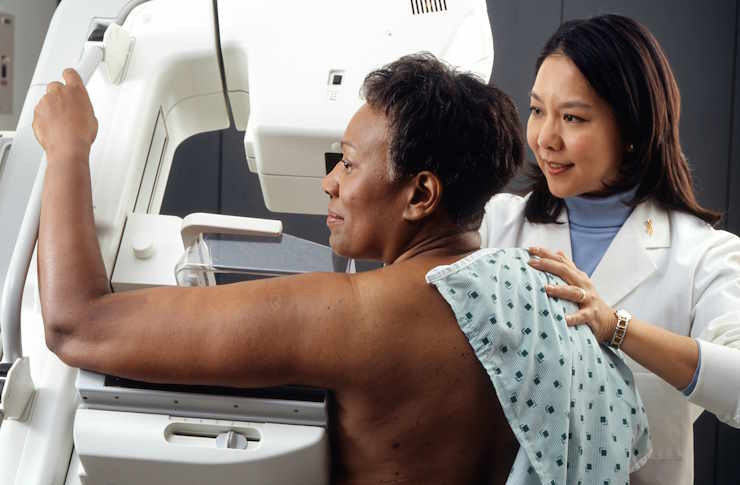
Cancer Treatment in 2026: Personalized Care and Advanced Therapies in the U.S
In 2026, cancer treatment in the United States is more personalized and advanced than ever before. From precision medicine and targeted therapies to immunotherapy and minimally invasive procedures, patients now have more informed choices to manage their care while maintaining quality of life.
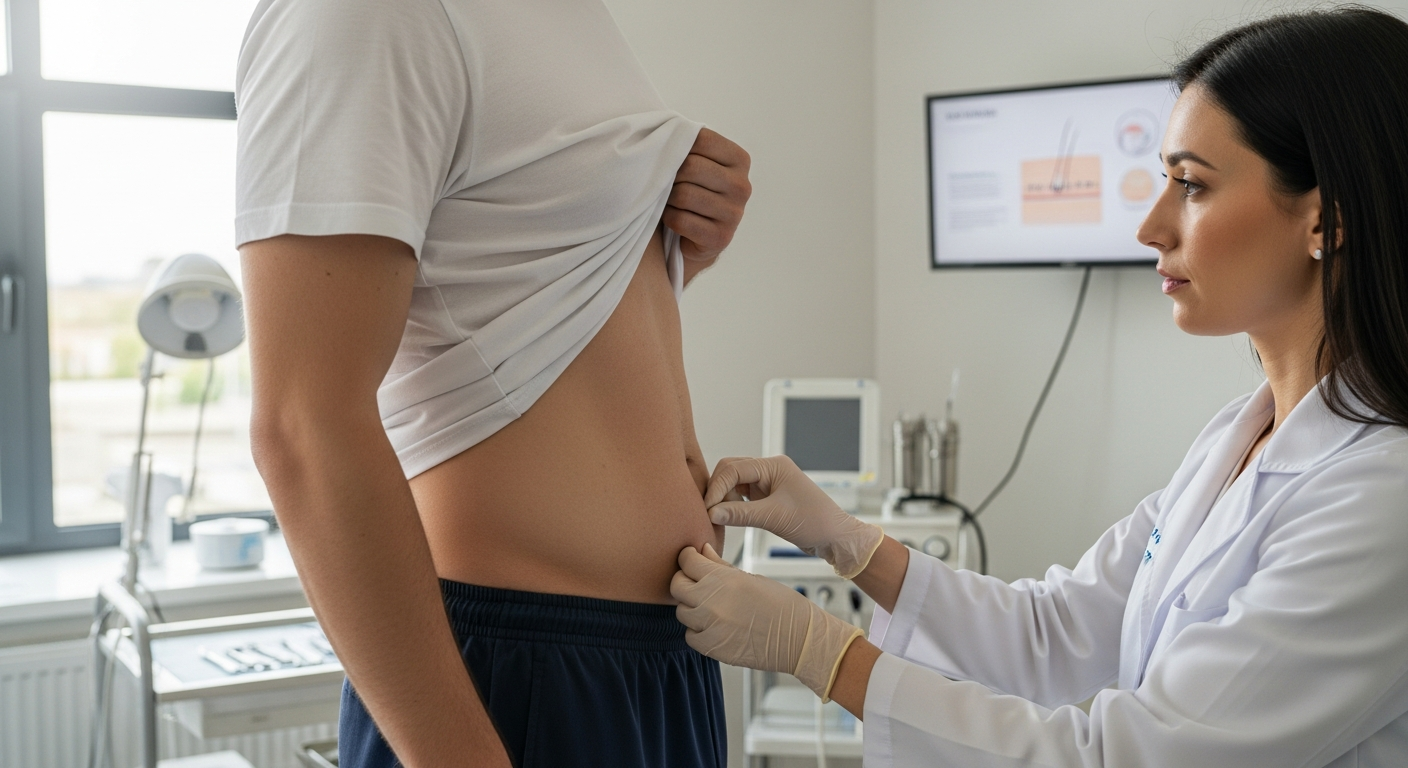
Cancer Treatment in 2026: Personalized Care and Advanced Therapies in the U.S
Across the United States, cancer treatment in 2026 increasingly combines cutting edge science with close attention to each person’s unique medical situation and preferences. Instead of one size fits all regimens, care teams now draw on genetic information, advanced imaging, and new medicines to design more precise plans. At the same time, there is growing emphasis on managing side effects, supporting mental health, and helping people maintain as much normalcy as possible during and after treatment.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Modern cancer treatment options in the U.S.
People diagnosed with cancer in the U.S. today usually encounter a mix of traditional and modern options. Core treatments still include surgery, radiation therapy, and chemotherapy, but how and when these are used has become far more individualized. For example, chemotherapy doses may be adjusted based on kidney or liver function, and radiation fields are shaped more precisely to spare nearby healthy tissues.
Many cancer centers now discuss treatment within multidisciplinary teams that include medical oncologists, surgeons, radiation oncologists, radiologists, pathologists, and supportive care specialists. This team approach helps align treatment choices with tumor type, stage, genetic features, other health conditions, and personal goals. Clinical trials are also a key part of the landscape, giving some patients access to new drugs, new combinations, and novel ways of delivering existing therapies.
Precision medicine and genetic testing
Precision medicine aims to match the right treatment to the right person at the right time. In cancer care, this often begins with testing tumor samples for specific genetic changes, sometimes called biomarkers. These changes do not usually come from parents but arise in the cancer cells themselves. Finding them can reveal how the tumor grows and which drugs are more likely to work.
In 2026, many people with lung, breast, colorectal, melanoma, and several blood cancers routinely receive molecular or genomic testing as part of their diagnostic workup. When a targetable mutation is found, doctors may recommend a targeted therapy designed to block that pathway. There is also increasing use of broader genomic panels that survey many genes at once, which can reveal rare alterations that point toward specific clinical trials.
Genetic testing of healthy cells, often through blood or saliva, may be offered when there is concern about inherited cancer risk. These results can guide screening schedules and prevention strategies for individuals and their families. Because genetic information is complex and sensitive, counseling by trained professionals is strongly encouraged before and after testing.
Emerging therapies: immunotherapy and targeted drugs
Immunotherapy has become one of the most visible advances in modern cancer care. Certain immunotherapies, such as checkpoint inhibitors, work by helping immune cells recognize and attack cancer more effectively. These drugs are now used for several cancers, including some types of lung cancer, melanoma, kidney cancer, bladder cancer, and others, often either alone or combined with chemotherapy or targeted therapy.
Targeted therapies focus on specific molecules or pathways that cancer cells rely on to grow and survive. Examples include drugs that block hormone signaling in some breast and prostate cancers, or medicines that interrupt growth signals in tumors with particular genetic mutations. Many targeted medicines are taken by mouth, sometimes for extended periods, which can allow treatment outside the hospital but also requires consistent monitoring for side effects.
Researchers are also developing cell based therapies, including certain types of engineered immune cell treatments, and new antibody based drugs that deliver toxic payloads directly to tumor cells. While these approaches are not appropriate for every person or every cancer type, they add important options for some people whose disease has not responded to earlier treatments.
Minimally invasive procedures and side effects
Minimally invasive techniques are increasingly used for both diagnosis and treatment. Examples include laparoscopic and robotic assisted surgeries that use small incisions and cameras, image guided biopsies, and procedures such as radiofrequency ablation or cryoablation that destroy tumors with heat or cold. For suitable patients and tumor locations, these methods may reduce hospital stays, blood loss, and recovery time compared with traditional open surgery.
Radiation therapy has also become more precise, with technologies that shape beams around the tumor and adjust for movement as a person breathes or swallows. This precision can help limit exposure to surrounding tissues. In parallel, supportive medicines such as modern anti nausea drugs, growth factors, and topical treatments for skin reactions have made many side effects more manageable than in the past, though they cannot eliminate them entirely.
Despite improvements, side effects remain a central concern in cancer care. Discussions between patients and clinicians often cover potential short term issues like fatigue, nausea, and hair loss, as well as long term effects on heart health, fertility, cognition, and bone strength. Shared decision making helps balance the hoped for benefits of treatment with its risks and impact on daily life.
Supportive care and lifestyle choices
Supportive care, sometimes called palliative care, has gained wider recognition as an essential part of high quality cancer treatment. It focuses on relieving symptoms, managing stress, and supporting emotional and spiritual well being, regardless of whether the cancer is early stage or advanced. Supportive care teams may include doctors, nurses, social workers, dietitians, physical and occupational therapists, and mental health professionals.
Lifestyle choices can also influence how people tolerate treatment and how they feel day to day. Many care teams encourage regular, gentle physical activity when possible, as it can help with fatigue, mood, and physical function. Nutritional guidance aims to maintain strength and manage issues such as taste changes or difficulty swallowing. Smoking cessation, limiting alcohol intake, and following individualized exercise and sleep plans are commonly recommended elements of comprehensive care when medically appropriate.
Emotional and social support matter as well. Counseling, peer groups, online communities, and family or caregiver involvement can help people navigate uncertainty, make complex decisions, and adjust to life during and after treatment. Survivorship programs, which focus on long term follow up, late effect monitoring, and healthy living plans, are becoming more common across the country.
Looking ahead for cancer treatment in 2026 and beyond
By 2026, cancer treatment in the U.S. increasingly reflects an approach that is both scientifically sophisticated and deeply personal. Precision testing, immunotherapy, targeted medicines, and minimally invasive techniques expand the menu of options, while supportive and palliative care emphasize symptom relief and overall well being. Even with these advances, decisions remain highly individual, shaped by the type and stage of cancer, available evidence, and personal priorities. Ongoing research, clinical trials, and improvements in access to high quality care will continue to influence how cancer is treated in the years to come.