Early Signs and Causes of Scalp Psoriasis: What You Should Know in 2026
Scalp psoriasis can look like ordinary flaking at first, but it often has distinct patterns such as persistent itching, thick scale, and redness that returns even after routine hair washing. Understanding early clues, likely triggers, and common look-alikes can help you have more informed conversations with a clinician and reduce avoidable irritation.
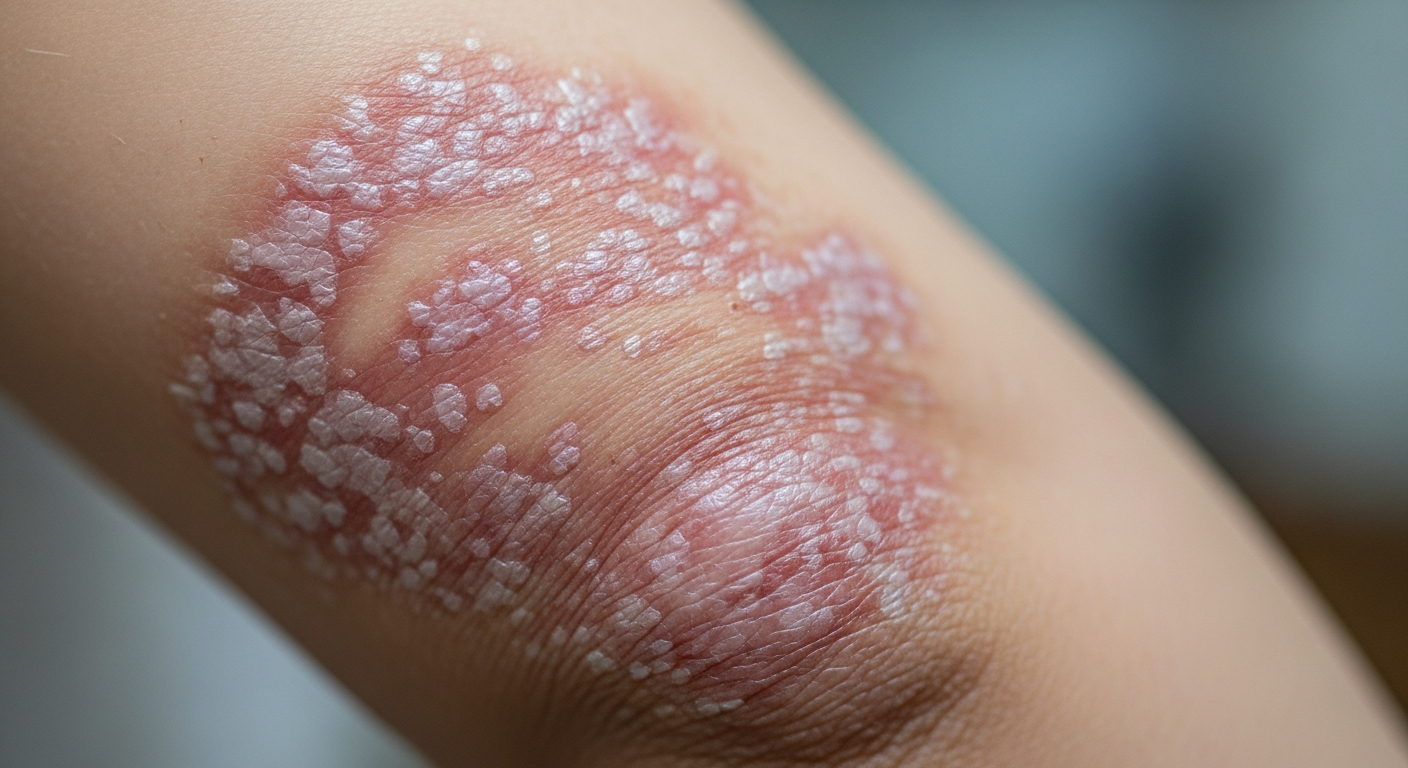
Patchy scaling on the scalp is common, but scalp psoriasis tends to be more persistent and inflammatory than everyday dryness. In 2026, clinicians still recognize it as a chronic immune-mediated skin condition that can wax and wane with triggers such as stress, infections, or irritating hair practices. Knowing what to look for, what may be driving it, and how it is typically assessed can reduce confusion and help you avoid worsening irritation.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Early Signs of Scalp Psoriasis to Watch For
Early scalp psoriasis often starts as well-defined pink-to-red patches with a silvery or white scale that clings to the skin rather than falling away easily. Itching, burning, or soreness may appear before heavy flaking does. Some people notice scaling that extends slightly beyond the hairline onto the forehead, behind the ears, or the back of the neck. Scratching can lead to pinpoint bleeding or tender areas, which may signal inflamed plaques rather than simple dryness.
What Causes Scalp Psoriasis?
Scalp psoriasis is generally understood as an immune-driven condition with a strong genetic component. Instead of skin cells shedding at a typical pace, inflammatory signaling speeds up cell turnover, causing buildup and scale. While it is not contagious, flare-ups can be influenced by triggers such as psychological stress, certain infections, skin injury (including aggressive scratching), smoking, or heavy alcohol use. Some medications may also worsen psoriasis in certain people, so medication history is often part of clinical evaluation.
Scalp Psoriasis vs. Dandruff: Key Differences
Dandruff usually refers to flaking from a non-psoriatic cause such as seborrheic dermatitis or irritation, and it often produces looser, greasy, yellow-white flakes with less sharply bordered redness. Scalp psoriasis more often creates thicker, drier scale and more clearly defined plaques that may extend beyond the hairline. Itch can occur in both, but psoriasis is more likely to involve other body sites (elbows, knees, nails) or a personal/family history of psoriasis. Because overlap can happen, a clinician may consider both conditions when symptoms persist.
How Scalp Psoriasis Is Evaluated and Managed
Diagnosis is typically clinical, based on appearance, distribution, symptoms, and whether similar plaques exist elsewhere. Clinicians may ask about nail changes, joint pain or stiffness, recent infections, and family history. Management often combines gentle scalp care (minimizing picking and harsh friction) with targeted therapies chosen by severity, hair type, and lifestyle. Options may include medicated shampoos, topical anti-inflammatory prescriptions, and, for more extensive disease, treatments that address inflammation more broadly.
| Provider Name | Services Offered | Key Features/Benefits |
|---|---|---|
| American Academy of Dermatology (AAD) | Dermatologist directory and education | Helps locate board-certified dermatologists and understand common skin conditions |
| National Psoriasis Foundation (NPF) | Patient education and support resources | Practical guidance for living with psoriasis and preparing for clinical visits |
| Teladoc Health | Telehealth medical visits (availability varies by state) | Convenient access for initial assessment and follow-up when appropriate |
| Amwell | Telehealth visits (availability varies by state) | Virtual care options that may support triage and ongoing management |
In many cases, a primary care clinician can start initial therapy and refer to dermatology if symptoms are severe, uncertain, or not improving. If the diagnosis is unclear, a clinician may consider scalp culture or, less commonly, a skin biopsy. Treatment plans often focus on reducing inflammation and scale while protecting the scalp barrier. Your clinician may also discuss trigger tracking and realistic expectations, since improvement can take time and maintenance strategies are common.
Potential Complications if Left Unmanaged
When scalp psoriasis is left unmanaged, persistent inflammation and scratching can cause skin breaks, pain, and secondary infection risk. Thick scale can be socially distressing and may disrupt sleep when itching is intense. Some people experience temporary hair shedding related to inflammation or mechanical trauma from picking; hair typically regrows when irritation is controlled, but ongoing damage can prolong shedding. Importantly, psoriasis can be associated with broader health considerations, including psoriatic arthritis, so new joint pain, swelling, or morning stiffness warrants medical evaluation.
Scalp psoriasis can resemble dandruff or irritation, but its hallmark is persistent, well-defined inflammatory scaling that often follows recognizable triggers. Paying attention to early patterns, possible causes, and coexisting signs on skin or nails can make evaluation more straightforward. A practical approach usually combines gentle scalp habits with clinician-guided therapies, aiming for symptom control and fewer flare-ups over time.