Early Signs and Causes of Scalp Psoriasis: What You Should Know in 2026
Scalp psoriasis affects millions of people worldwide, causing uncomfortable symptoms that can significantly impact daily life. This chronic autoimmune condition manifests as red, scaly patches on the scalp, often accompanied by itching and flaking. Understanding the early warning signs and underlying causes can help individuals seek appropriate medical guidance sooner rather than later. While scalp psoriasis shares some similarities with common dandruff, the two conditions have distinct characteristics that require different approaches to management.
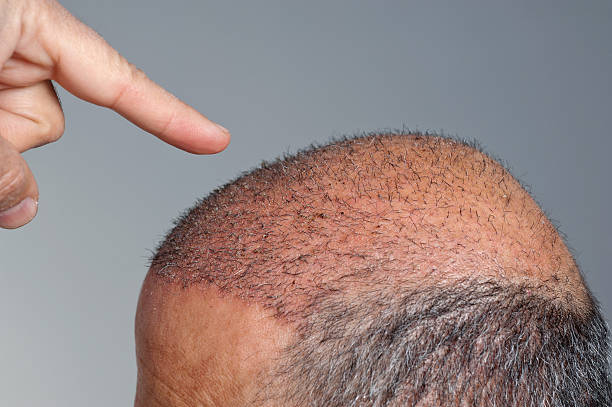
Scalp psoriasis represents one of the most common forms of psoriasis, a chronic autoimmune skin condition that can affect people of all ages. Unlike temporary scalp irritations, this condition involves the immune system mistakenly attacking healthy skin cells, leading to rapid cell turnover and the characteristic symptoms many people experience.
Early Signs of Scalp Psoriasis to Watch For
Recognizing the initial symptoms of scalp psoriasis can make a significant difference in managing the condition effectively. The earliest signs often include persistent itching that seems more intense than typical scalp irritation. Red, inflamed patches may appear on various areas of the scalp, sometimes extending beyond the hairline to the forehead, neck, or behind the ears.
Silvery-white scales typically develop on these red patches, creating a distinctive appearance that differs from regular dandruff. Hair loss may occur in affected areas, though this is usually temporary when proper care is provided. Many individuals also report tenderness or soreness in the affected regions, particularly when touching or brushing the hair.
What Causes Scalp Psoriasis?
The development of scalp psoriasis involves complex interactions between genetic predisposition and environmental factors. Research indicates that individuals with family members who have psoriasis face a higher likelihood of developing the condition themselves. The immune system plays a central role, as T-cells mistakenly identify healthy skin cells as threats and trigger an inflammatory response.
Stress often serves as a significant trigger, potentially causing flare-ups or worsening existing symptoms. Certain medications, infections, and injuries to the scalp can also initiate or exacerbate the condition. Weather changes, particularly cold and dry conditions, frequently contribute to symptom severity. Lifestyle factors such as smoking and excessive alcohol consumption may increase the risk of developing scalp psoriasis.
Scalp Psoriasis vs. Dandruff: Key Differences
Distinguishing between scalp psoriasis and common dandruff requires careful observation of specific characteristics. Dandruff typically produces smaller, white or yellowish flakes that fall easily from the scalp, while psoriasis creates thicker, silvery scales that adhere more firmly to the skin. The underlying skin in psoriasis cases appears distinctly red and inflamed, whereas dandruff usually involves less dramatic skin changes.
Itching intensity also differs between the two conditions. Psoriasis often causes more severe, persistent itching that may interfere with sleep and daily activities. The location of symptoms can provide additional clues, as psoriasis frequently extends beyond the scalp to other body areas, while dandruff remains confined to the scalp region.
How Scalp Psoriasis Is Evaluated and Managed
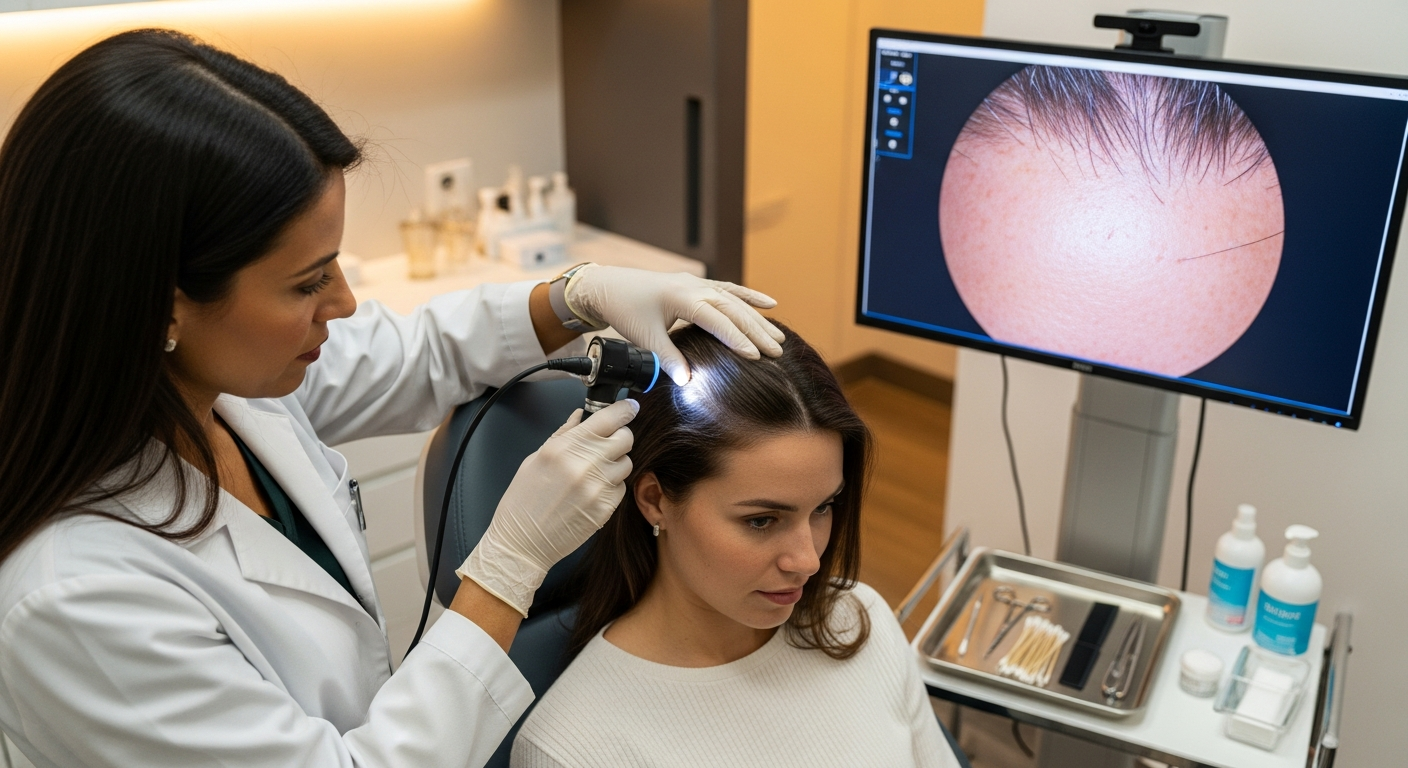
Healthcare professionals typically diagnose scalp psoriasis through visual examination and medical history review. In some cases, a small skin sample may be collected for microscopic analysis to confirm the diagnosis and rule out other conditions. The evaluation process often includes questions about family history, potential triggers, and symptom patterns.
Management approaches vary depending on symptom severity and individual response to different treatments. Topical medications containing corticosteroids, vitamin D analogs, or tar-based compounds are commonly prescribed for mild to moderate cases. More severe conditions may require systemic medications or light therapy treatments. Regular follow-up appointments help monitor progress and adjust treatment plans as needed.
Potential Complications if Left Unmanaged
Without appropriate management, scalp psoriasis can lead to several complications that extend beyond cosmetic concerns. Persistent scratching may result in secondary bacterial infections, creating additional health challenges that require separate treatment approaches. Temporary hair loss can become more extensive or prolonged when inflammation remains uncontrolled.
The psychological impact of visible symptoms can significantly affect quality of life, potentially leading to social anxiety or self-esteem issues. Sleep disturbances from intense itching may contribute to fatigue and decreased productivity. In some individuals, untreated scalp psoriasis may progress to affect other body areas or develop into more severe forms of the condition.
The chronic nature of scalp psoriasis means that symptoms may fluctuate over time, with periods of improvement followed by flare-ups. Understanding this pattern helps individuals develop realistic expectations and maintain consistent care routines even during symptom-free periods.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.