Scalp Psoriasis Treatment in 2026: What’s New, What Works, and What to Know
Scalp psoriasis, a common chronic autoimmune condition, manifests as red, scaly patches on the scalp, often accompanied by itching and discomfort. While it can be a challenging condition to manage, advancements in dermatological science continue to offer more effective and targeted treatment options. As we look towards 2026, understanding the latest developments, established therapies, and how they integrate into a comprehensive care plan is crucial for individuals seeking relief and improved quality of life. This article explores the current landscape of scalp psoriasis treatment, from foundational topical applications to cutting-edge systemic therapies.
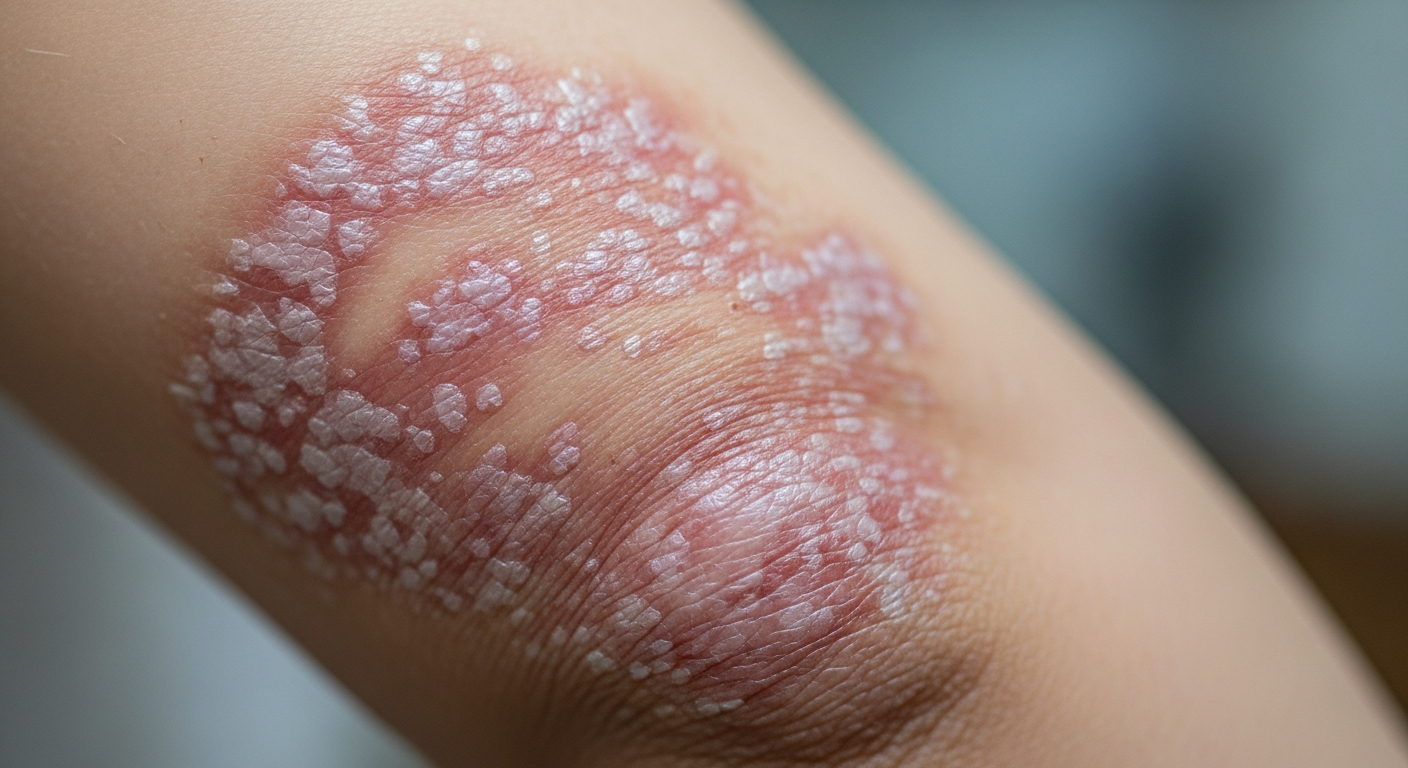
Understanding Scalp Psoriasis
Scalp psoriasis is a distinct form of psoriasis that primarily affects the scalp, though it can extend to the forehead, back of the neck, and behind the ears. It is characterized by thick, silvery-white scales over well-defined red patches, which can be itchy, painful, and sometimes lead to temporary hair loss. This condition is not contagious and stems from an overactive immune system that accelerates the skin cell production cycle. While the exact cause remains unknown, it is believed to involve a combination of genetic predisposition and environmental triggers. Effective management often requires a multifaceted approach tailored to the individual’s specific symptoms and disease severity.
Topical Treatments: Still the First Line of Defense
For many individuals with mild to moderate scalp psoriasis, topical treatments remain the cornerstone of therapy. These medications are applied directly to the affected areas of the scalp and work to reduce inflammation, slow down skin cell growth, and remove scales. Common topical agents include corticosteroids, which are potent anti-inflammatory drugs available in various strengths and formulations like solutions, foams, gels, and shampoos. Other effective topical options include vitamin D analogues (such as calcipotriene), which help regulate skin cell production, and coal tar, known for its ability to reduce scaling and itching. Salicylic acid is often used to soften and remove thick scales, allowing other medications to penetrate more effectively. Newer topical formulations continue to emerge, aiming for improved efficacy and reduced side effects.
Biologic Therapies: Targeted Relief for Moderate to Severe Disease
For individuals with moderate to severe scalp psoriasis, especially when topical treatments have proven insufficient or the condition significantly impacts quality of life, biologic therapies represent a significant advancement. These medications are administered via injection or intravenous infusion and work by targeting specific components of the immune system involved in the inflammatory process of psoriasis. Unlike traditional systemic medications that broadly suppress the immune system, biologics offer a more precise approach, leading to substantial improvements in skin clearance for many patients. Examples include TNF-alpha inhibitors, IL-17 inhibitors, and IL-23 inhibitors, each designed to block different inflammatory pathways. The selection of a specific biologic depends on various factors, including the patient’s overall health, other medical conditions, and previous treatment responses. These therapies are typically prescribed and monitored by a dermatologist.
Light Therapy and At-Home Devices
Light therapy, also known as phototherapy, involves exposing the scalp to specific wavelengths of ultraviolet (UV) light, typically UVB. This treatment works by slowing down the rapid growth of skin cells and reducing inflammation. It is often administered in a clinical setting under the supervision of a dermatologist, either through targeted light units or full-body booths for more widespread psoriasis. For localized scalp psoriasis, specialized light combs or handheld devices can deliver UV light directly to the scalp, minimizing exposure to other areas of the body. In recent years, there has been an increase in the availability of at-home phototherapy devices, which can be a convenient option for some patients under strict medical guidance. However, it is crucial to use these devices responsibly and according to a dermatologist’s instructions to ensure safety and effectiveness, as improper use can lead to burns or other skin damage.
Managing scalp psoriasis involves a range of treatments, and understanding the potential costs associated with these therapies is an important consideration for patients. The expenses can vary significantly based on the type of treatment, insurance coverage, and whether generic or brand-name medications are used. Topical treatments are generally the most affordable, while biologics represent a substantial investment due to their complex manufacturing process and targeted action.
| Product/Service Category | Provider Type | Cost Estimation (USD per month) |
|---|---|---|
| Over-the-counter topicals | Pharmacy/Drugstore | $10 - $50 |
| Prescription topicals | Pharmacy (with prescription) | $30 - $300 |
| In-office light therapy | Dermatology clinic | $50 - $200 per session |
| At-home light therapy device | Medical supply/Specialty retailer | $300 - $1,500 (one-time purchase) |
| Biologic therapies | Specialty pharmacy (with prescription) | $2,000 - $10,000+ |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Looking ahead to 2026, the landscape of scalp psoriasis treatment continues to evolve, offering new hope for individuals seeking effective management. From established topical therapies to advanced biologic medications and accessible light therapy options, the array of treatments allows for highly individualized care plans. Collaboration with a healthcare professional is key to navigating these options, ensuring that the chosen approach aligns with an individual’s specific needs, disease severity, and lifestyle, ultimately leading to better control of symptoms and an improved quality of life.




